Anatomy of Turf Toe

The simplest definition of turf toe is that it is a sprain of the main joint of the big toe. It happens when the toe is forcibly bent up into hyperextension, such as when pushing off into a sprint and having the toe get stuck flat on the ground.
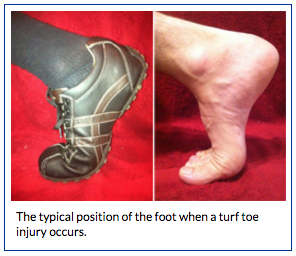 Sprains of the big toe joint became especially prevalent in American football players after artificial turf became more common on playing fields – hence the term “turf toe.” Artificial turf is a harder surface than grass and does not have much “give” when forces are placed on it.
Sprains of the big toe joint became especially prevalent in American football players after artificial turf became more common on playing fields – hence the term “turf toe.” Artificial turf is a harder surface than grass and does not have much “give” when forces are placed on it.
Although often associated with football, turf toe occurs in a wide range of sports and activities.
Anatomy
The big toe is made up of two joints. The largest of the two is the metatarsophalangeal joint (MTP), where the first long bone of the foot (metatarsal) meets the first bone of the toe (phalanx). In turf toe, the MTP joint is injured.
The joint is surrounded by important structures that hold it in place and prevent it from dislocating. Together these structures are referred to as the “plantar complex.”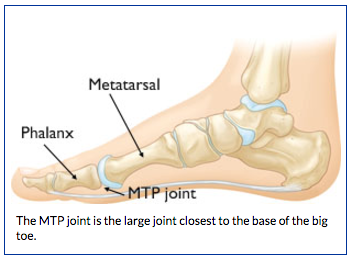
- Plantar plate. This thick, fibrous tissue under the MTP joint prevents the big toe from bending too far (dorsiflexion).
- Collateral ligaments. Located on each side of the big toe, collateral ligaments connect the phalanx bone to the metatarsal and prevent the toe from going too far side-to-side.
- Flexor hallucis brevis. This tendon runs under the first metatarsal bone and attaches to the phalanx. It provides strength and stability to the big toe during push-off motions.
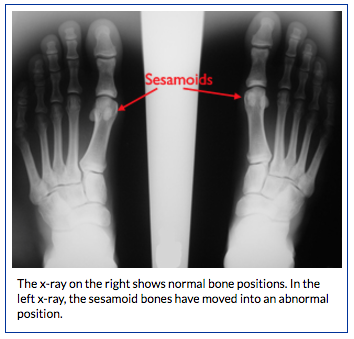
- Sesamoids. These two small bones are enveloped in the flexor hallucis tendon, and help it to move more easily. In addition, the sesamoids provide stability to the MTP joint by helping to bear weight placed on the forefoot.
Description
The term “turf toe” refers to an injury of any soft tissue structure in the plantar complex, such as the plantar plate or a collateral ligament. These injuries can vary in severity — from stretching of the soft tissue to partial tearing, and even total dislocation of the MTP joint.
To help them plan treatment for turf toe, doctors grade the injuries from 1 to 3 – mild to severe.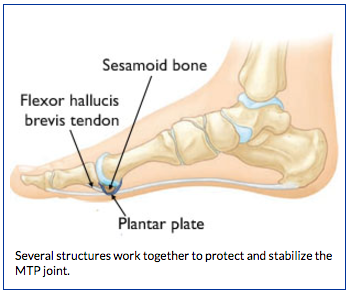
- Grade 1. The plantar complex has been stretched causing pin-point tenderness and slight swelling.
- Grade 2. A partial tearing of the plantar complex causes more widespread tenderness, moderate swelling, and bruising. Movement of the toe is limited and painful.
- Grade 3. The plantar complex is completely torn causing severe tenderness, severe swelling, and bruising. It is difficult and painful to move the big toe.
Cause
Turf toe can occur in any sport or activity when the forefoot is fixed on the ground, the heel is raised, and a force pushes the big toe into hyperextension.
These injuries most often occur among American football players on artificial grass. Artificial surfaces tend to be harder and less shock absorbent. In addition, the athletic shoes designed for artificial surfaces are softer and more flexible, providing the athlete with more agility, but much less stability in the forefoot.
First Aid Treatment
The RICE protocol is effective for most sports-related injuries when they first occur. RICE stands for Rest, Ice, Compression, and Elevation.
- Rest. Take a break from the activity that caused the injury and avoid walking or putting weight on your foot.
- Ice. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly to the skin.
- Compression. To help prevent additional swelling, wear an elastic compression bandage.
- Elevation. To reduce swelling, recline when you rest, and put your leg up higher than your heart.
In addition, over-the-counter anti-inflammatory medications, such as ibuprofen, can help provide symptom relief.
Depending upon the severity of your injury, seek a doctor’s care immediately or if your symptoms persist. Before your appointment, try to identify exactly what happened when the injury occurred. This information can help your doctor to diagnose your injury and plan your treatment.
Doctor Examination
Medical History and Physical Examination
During your appointment, your doctor will talk to you about your general health and your toe symptoms, and ask you to describe how you injured your toe.
During the physical examination of your foot, your doctor will check for swelling, bruising, and the range of motion of your MTP joint. Your doctor will bend your toe up, move it up and down, and side to side, looking for instability that might suggest a tear in the plantar complex. He or she may also perform the same range of motion tests on your healthy toe as a comparison.
Examining the range of motion in your toe may be painful. If needed, your doctor may inject the area with a numbing medicine prior to the range-of-motion tests.
Imaging Tests
Other tests that your doctor may order to help confirm your diagnosis include:
- X-rays. This imaging test creates clear pictures of dense structures, like bone. Although the plantar complex is made up of different soft tissues, your doctor may order x-rays to make sure there are no other problems in your toe. These may include small bony pull-off fractures where the plantar complex attaches to the bones, and fractures or movement of the two small sesamoid bones.
- Magnetic resonance imaging (MRI) scan. These studies can create better images of soft tissue and can show soft tissue and cartilage injuries. An MRI scan may be useful in Grade 2 and 3 injuries or when abnormalities are noted on the x-rays.
Treatment
 Nonsurgical Treatment
Nonsurgical Treatment
Most cases of turf toe are treated without surgery. Nonsurgical treatment is determined by the grade of the injury.
- Grade 1. The RICE protocol is recommended for this type of injury: Rest, ice, compression, and elevation. Taping the big toe to the smaller toes will restrict motion. Non-steroidal anti-inflammatory medications may relieve pain and swelling.
Pain is usually tolerable and an athlete can continue sports participation using a stiff-soled shoe. Orthotics, such as a thin, graphite shoe insert with a rigid forefoot component, can reduce stress on the plantar plate and provide stability. - Grade 2. To keep the MTP joint immobilized, a walking boot may be prescribed for up to a week if needed. Afterwards, these injuries are managed with a taping regimen and the Grade 1 treatments discussed above.
In most cases, an athlete with a Grade 2 injury needs 3 to 14 days of rest before returning to play.  Grade 3. These more severe injuries are most often treated with immobilization for several weeks. The athlete may wear a walking boot or be put in a cast that keeps the big toe in a partially pointed down position. As the injury heals, treatment will gradually step down to Grade 2 and then to Grade 1.
Grade 3. These more severe injuries are most often treated with immobilization for several weeks. The athlete may wear a walking boot or be put in a cast that keeps the big toe in a partially pointed down position. As the injury heals, treatment will gradually step down to Grade 2 and then to Grade 1.
Physical therapy may be helpful and should be started as soon as symptoms allow. Specific exercises will help to stretch and strengthen the big toe. Early joint movement is essential for reducing or preventing joint stiffness.
Surgical Treatment
Surgery is not often necessary for treating turf toe. However, if your symptoms persist or your level of athletic play is affected, surgery may be an option. Doctors most often recommend surgery for larger Grade 3 injuries, such as:
- A severe tear of the plantar complex
- Fracture of the sesamoid
- Vertical instability (unusual up and down motion) of the MTP joint
- Loose bony chip in the joint
- Damage to the cartilage of the joint
- New or worsening bunion
The surgical procedure will vary according to the injury. The aim of surgery is to repair the soft tissues and restore the MTP joint motion so that normal function can be preserved.
Long-Term Outcomes
Turf toe injuries that are addressed early, typically heal fairly well.
A wide range of mild to moderate, but persistent symptoms — such as pain and joint stiffness — are the most common complications.
Potential long-term complications include lack of push-off strength, stiffness, bunion, and cocking up of the big toe.
BoulderCentre can help. Call us (303) 449-2730 and ask to see one of our foot and ankle specialists or choose from any one of our many surgical or general health practitioners.
Article courtesy of AAOS: American Academy of Orthopedic Surgeons.